World Glaucoma Week:
The Importance of Early Detection in Preventing Blindness

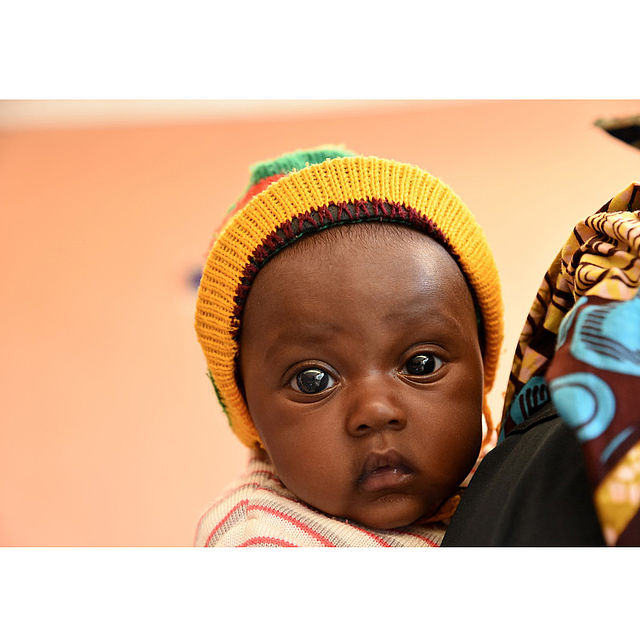
Yasmine received glaucoma treatment at a CBM partner eye hospital in Cameroon.
©CBM
Glaucoma is the most common cause of irreversible blindness worldwide.
Glaucoma Week, which this year runs from 12 to 18 March, aims to raise awareness and understanding of the importance of early detection of glaucoma.
According to the figures collected so far, CBM has supported 20,740 glaucoma surgeries in 2022 with implementing partners in 79 projects and 20 countries. In addition, one of our Eye Health Advisors Heiko Philippin has been working on a study to advance glaucoma treatment.
In many African countries, people come to eye centres only when glaucoma (caused by damage to the optic nerve, often due to increased eye pressure) is at an advanced stage and there is less chance of preserving vision and preventing irreversible blindness.
Glaucoma and its progression are diagnosed by testing the function of the eye and looking at changes in the optic nerve - a cable-like structure at the back of the eye made up of more than a million nerve fibres. In glaucoma, these fibres slowly die. This creates what ophthalmologists call a 'excavation', a central depression in the optic nerve head that increases in size as the disease progresses.
This diagnostic process is often performed using expensive equipment ( for example OCT imaging technology). The purchase of this equipment can sometimes drain financial resources in facilities where resources are already stretched.
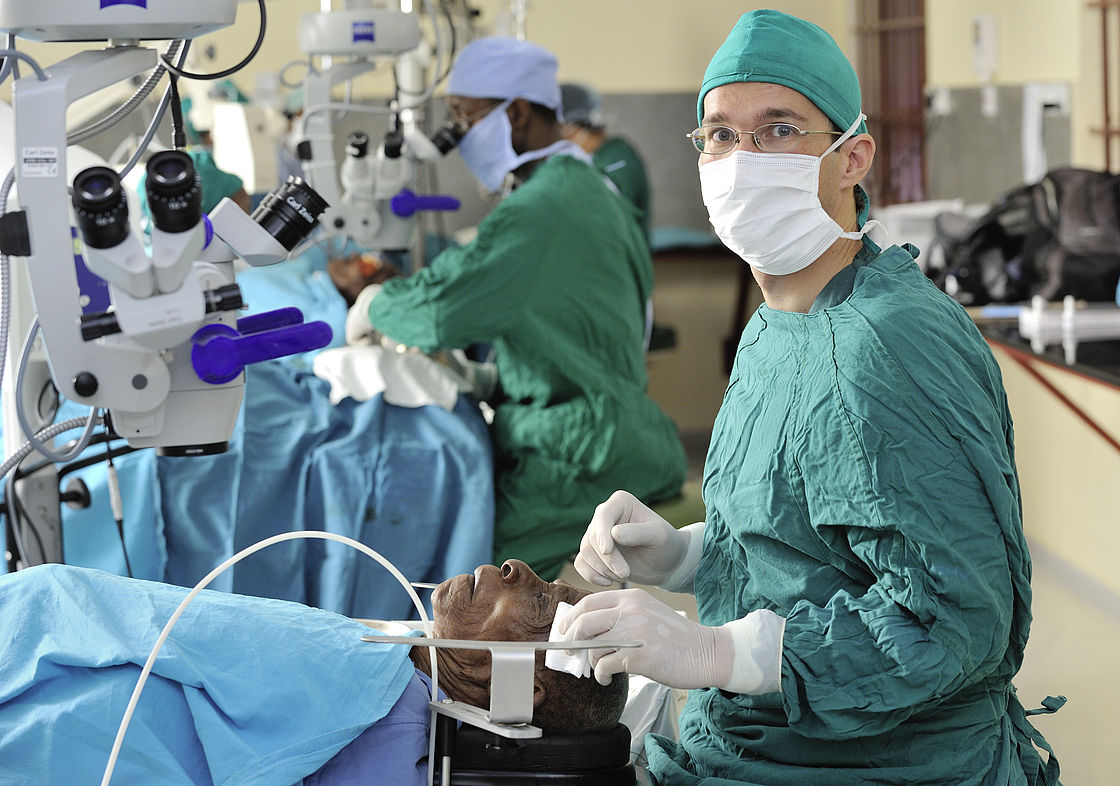
Dr. Heiko Philippin (ophthalmologist) during surgery in the operating theatre at Kilimanjaro Christian Medical Centre in Moshi, Tanzania.
CBM/argum/Einberger
Heiko Philippin, CBM Advisor on Eye Health and a Research Fellow at the London School of Hygiene and Tropical Medicine, who has worked in Tanzania for many years, recently conducted a study on several established scoring methods to describe these optic nerve changes without the use of diagnostic equipment.
The results of the study show that low-cost methods using a slit lamp or direct ophthalmoscope to screen and describe the optic nerve using a score can effectively detect the progression of the disease. Any deterioration can be compared with previous screenings. In patients where the disease is advanced, the scores still perform well. Heiko said:
"In patients in Tanzania with moderate and advanced glaucoma we were able to show that we can differentiate the stages of glaucoma using low-cost methods, including very advanced stages. In a scenario where resources are limited it may make sense therefore, to focus more on investing in treatment options such as lasers used to reduce pressure in the eye rather than expensive diagnostic tools. There is no clear evidence in the literature that the diagnostic machines currently do a better job to detect progression."
People are generally unaware of glaucoma and the importance of early detection. As long as the disease is identified before it affects the central visual field and monitored regularly, people can maintain good vision and live relatively unimpaired lives most of the time.
"In places with sufficient resources, people predominantly present early with the condition because people have access to eye care. But I have also worked in situations where I was just happy to catch someone before the glaucoma was very advanced. Our ageing population means that age-dependent eye conditions like glaucoma are likely to increase, but my hope is that if we are able to raise awareness and strengthen health systems, more people will come to us and be detected earlier. With the use of technology such as mobile phone apps that enable eye screening to take place in communities and better training of eye specialists at the primary and secondary level, we will be able to offer good treatment to more people and prevent more irreversible blindness from glaucoma."
The importance of early detection...
Pauline noticed that her daughter's left eye was slightly bigger than her right. Worried that this might affect her vision in the future, Pauline made the journey to CBM partner Acha Eye Hospital in Bafoussam, Cameroon.
Yasmine was diagnosed with congenital glaucoma, which can lead to blindness if left untreated. Because Yasmine was diagnosed early, she received treatment to control the pressure in her eye and preserve her vision.
Read Heiko Philippin’s paper in the British Journal of Ophthalmology